Understanding Ultrasound-Guided Thyroid Biopsy
Ultrasound-guided thyroid biopsies are crucial for evaluating nodules, often utilizing specific CPT codes like 60008 for accurate billing and procedure identification.
What is a Thyroid Biopsy?
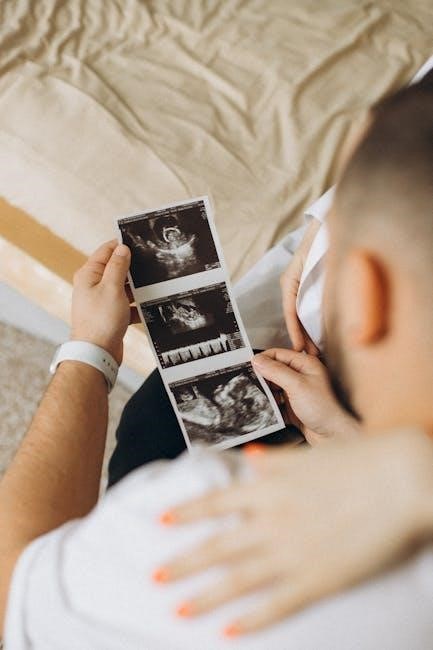
A thyroid biopsy is a procedure to remove a small sample of tissue from the thyroid gland for examination under a microscope. This is typically performed when a nodule is discovered during a physical exam or imaging study, like an ultrasound. The primary goal is to determine if the nodule is benign (non-cancerous) or malignant (cancerous).
Ultrasound guidance is frequently used to ensure accurate needle placement, especially for small or deeply located nodules. The CPT code 60008 is commonly associated with this procedure, representing the ultrasound guidance for percutaneous needle placement. Proper coding is essential for accurate billing and record-keeping, reflecting the complexity and precision involved in diagnosing thyroid conditions.
The Role of Ultrasound in Thyroid Biopsies
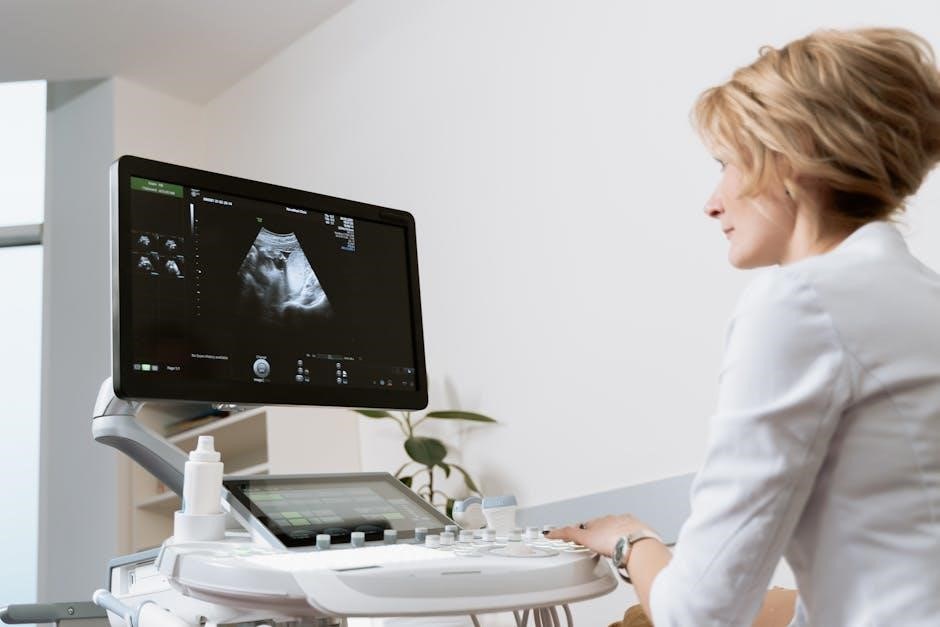
Ultrasound serves as the cornerstone of modern thyroid biopsy procedures, providing real-time visualization of the thyroid gland and nodules. This imaging modality allows physicians to precisely guide the biopsy needle to the target area, enhancing accuracy and minimizing the risk of complications. It’s considered an extension of the physical exam, offering detailed insights.
The use of ultrasound directly impacts CPT coding; specifically, code 60008 is utilized when ultrasound guidance is employed during the biopsy. This code acknowledges the skill and technology involved in performing an ultrasound-guided procedure, ensuring appropriate reimbursement for healthcare providers. Accurate ultrasound assessment helps determine if a biopsy is even necessary.
CPT Codes for Ultrasound-Guided Thyroid Biopsy
CPT code 60008 is central to billing for ultrasound-guided thyroid biopsies, reflecting the procedure’s complexity and the use of imaging technology.
Primary CPT Code: 60008
CPT code 60008 specifically represents ultrasound guidance for percutaneous needle placement for biopsy or aspiration of the thyroid gland. This code encompasses the entire process, from initial ultrasound imaging to the actual needle insertion and sample collection. It’s the foundational code used when reporting this common diagnostic procedure.
Proper application of 60008 is vital for accurate reimbursement. It’s important to note that this code doesn’t inherently include the pathological examination of the collected sample; that’s typically billed separately with relevant pathology CPT codes. Understanding the scope of 60008 ensures correct coding and avoids claim denials, streamlining the billing cycle for healthcare providers.
Modifier Usage with 60008
CPT code 60008 often requires modifiers to accurately reflect the services rendered. Modifier -59 (Distinct Procedural Service) is crucial when multiple procedures are performed at the same session, preventing bundled payment denials. For example, if a separate lesion is biopsied, -59 clarifies it’s not an integral part of the initial biopsy.

Modifier -26 (Professional Component) may be appended when only the physician’s professional services are billed, excluding the technical component (equipment, supplies). Correct modifier usage is paramount for compliant billing, ensuring appropriate reimbursement for the specific services provided during the ultrasound-guided thyroid biopsy procedure.
Modifier -59 (Distinct Procedural Service)
Modifier -59 signifies that a procedure performed alongside CPT 60008 (Ultrasound-guided thyroid biopsy) is distinct and not inherent to the primary service. It’s essential when multiple biopsies are conducted on separate thyroid nodules during the same session. Without -59, the second biopsy might be incorrectly denied as bundled into the initial procedure.
Proper application of -59 requires clear documentation demonstrating each biopsy targeted a unique lesion. This prevents claim rejections and ensures accurate reimbursement for all legitimately performed services. Accurate coding with modifier -59 is vital for compliant billing practices in ultrasound-guided thyroid biopsies.
Modifier -26 (Professional Component)
Modifier -26 is appended to CPT 60008 (Ultrasound-guided thyroid biopsy) to identify the professional component of the service – specifically, the physician’s work, including image interpretation, needle guidance, and biopsy performance. This is crucial when the facility bills separately for the technical component, such as ultrasound equipment usage and supplies.
Using -26 ensures the physician receives appropriate reimbursement for their expertise. Accurate billing requires a clear separation between professional and technical aspects. Failing to utilize -26 when applicable can lead to underpayment or claim denials. Proper coding with modifier -26 is essential for compliant and accurate billing practices.
Indications for Ultrasound-Guided Thyroid Biopsy
Ultrasound-guided thyroid biopsies, often billed using CPT 60008, are indicated when evaluating thyroid nodules. These nodules can be palpable during a physical exam or discovered incidentally during imaging performed for unrelated reasons. Suspicious ultrasound features, like those suggesting malignancy, strongly warrant biopsy consideration.
Specifically, nodules exhibiting concerning characteristics – hypoechoic patterns, microcalcifications, or irregular margins – increase the likelihood of cancer. Guidelines are evolving, with AI assisting in risk stratification to reduce unnecessary procedures. Accurate CPT coding is vital when performing biopsies based on these indications.
Palpable Thyroid Nodules
When a thyroid nodule is detected through physical examination, an ultrasound-guided biopsy, frequently coded with CPT 60008, becomes a key diagnostic step. While many palpable nodules are benign, assessing their characteristics is crucial. Ultrasound helps determine if the nodule possesses features requiring further investigation.
The decision to biopsy isn’t solely based on palpability; ultrasound findings heavily influence it. Features like size, echogenicity, and margins guide the clinician. Proper documentation supporting the medical necessity, linked to the CPT code, is essential for accurate billing and reimbursement.
Thyroid Nodules Identified on Imaging
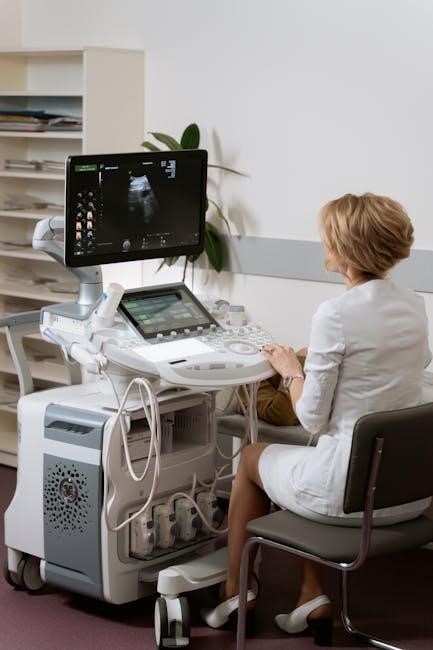
Incidental thyroid nodules discovered during imaging studies (like neck CTs or ultrasounds performed for other reasons) often necessitate further evaluation, typically with an ultrasound-guided biopsy coded as CPT 60008. These incidentally found nodules may not cause symptoms, but their potential for malignancy warrants investigation;
The size and characteristics observed on initial imaging dictate the need for a targeted biopsy. Ultrasound provides detailed visualization, guiding the needle to the suspicious area. Accurate CPT coding and detailed documentation of imaging findings are vital for justifying the procedure to insurance providers and ensuring appropriate reimbursement.
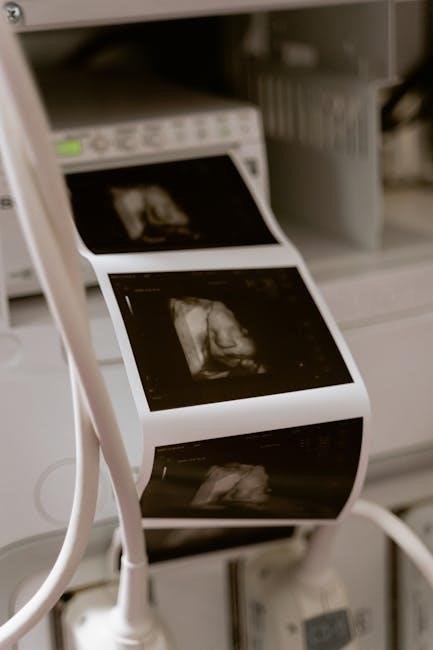
Suspicious Ultrasound Features
Certain ultrasound characteristics heighten concern for malignancy, prompting consideration of an ultrasound-guided thyroid biopsy, typically billed using CPT code 60008. These features include hypoechoic nodules, microcalcifications, and irregular margins, all suggesting a higher risk profile.
When these features are present, a biopsy is often recommended to obtain a tissue sample for pathological analysis. Proper documentation of these suspicious features is crucial for supporting the medical necessity of the procedure and ensuring accurate CPT coding. Detailed imaging reports are essential for both clinical decision-making and billing purposes.
Ultrasound Features Suggesting Malignancy
Identifying suspicious features on thyroid ultrasound is paramount in determining the need for a biopsy, often coded with CPT 60008. Key indicators include hypoechoic nodules – appearing darker than surrounding tissue – and the presence of microcalcifications, tiny calcium deposits within the nodule.
Irregular margins, signifying an uneven or poorly defined nodule border, also raise concern. These features don’t definitively confirm cancer, but significantly increase the probability, justifying further investigation via biopsy. Accurate documentation of these ultrasound findings is vital for appropriate CPT code assignment and reimbursement.
Hypoechoic Nodules
Hypoechoic nodules, appearing darker than the surrounding thyroid tissue on ultrasound, are frequently evaluated with a biopsy, typically billed using CPT code 60008. This characteristic suggests reduced blood flow and a potentially different tissue composition. While not always cancerous, they warrant closer scrutiny.
Radiologists consider hypoechogenicity alongside other features like size, shape, and margins when assessing risk. The decision to biopsy, and therefore utilize the CPT code, isn’t solely based on this finding. Detailed documentation of the nodule’s echogenicity is crucial for accurate coding and justifying the procedure’s medical necessity.
Microcalcifications
Microcalcifications – tiny calcium deposits within thyroid nodules – are a significant ultrasound finding often prompting a biopsy, coded with CPT code 60008. These small, punctate echoes raise suspicion for papillary thyroid carcinoma, the most common type of thyroid cancer.
However, not all microcalcifications indicate malignancy; their pattern and distribution are key. Radiologists carefully assess these features before recommending a biopsy. Proper documentation detailing the microcalcifications’ characteristics is essential for accurate CPT coding and supporting the medical necessity of the procedure. The presence of microcalcifications significantly influences the risk stratification process.
Irregular Margins
Irregular margins, observed during ultrasound, describe poorly defined or indistinct borders of a thyroid nodule, frequently leading to a biopsy coded as CPT 60008. Smooth, well-defined margins are generally benign, while irregular ones suggest potential invasiveness and a higher risk of malignancy.
This feature, alongside others, guides the decision to perform a fine needle aspiration. Detailed documentation of margin characteristics is crucial for accurate CPT coding and justifying the procedure’s medical necessity. Radiologists assess the shape and border definition to determine the need for further investigation, impacting patient management and treatment planning.
Pre-Procedure Preparation
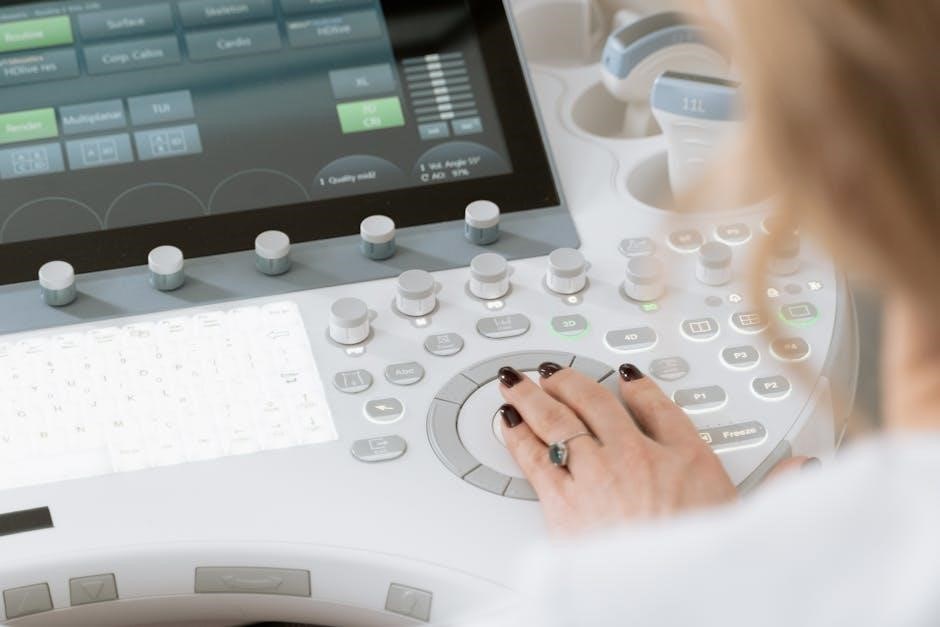
Prior to an ultrasound-guided thyroid biopsy, coded typically as CPT 60008, thorough patient preparation is essential. This includes a detailed review of the patient’s medical history, focusing on bleeding disorders and medications like anticoagulants. Obtaining informed consent is paramount, explaining the procedure, potential risks, and benefits.
Patients should understand the purpose of the biopsy and what to expect during and after the procedure. Accurate documentation of this process is vital for compliant CPT coding and reimbursement. Pre-procedure instructions often involve temporarily discontinuing blood thinners, if medically safe, to minimize bleeding risk.
Patient History and Medication Review
A comprehensive patient history is critical before an ultrasound-guided thyroid biopsy (often billed using CPT code 60008). Specifically, clinicians must identify any bleeding disorders or conditions affecting coagulation. A detailed medication review is equally important, with a focus on anticoagulants, antiplatelet drugs, and even certain supplements.
Understanding the patient’s medication list ensures appropriate pre-procedural management to minimize bleeding risks during the biopsy. Documenting this review thoroughly supports accurate CPT coding and demonstrates medical necessity. Any allergies, especially to iodine or local anesthetics, must also be carefully noted.
Informed Consent
Obtaining informed consent is paramount before proceeding with an ultrasound-guided thyroid biopsy, typically coded as CPT 60008. Patients must understand the procedure’s purpose, potential benefits – aiding in cancer diagnosis – and inherent risks, including bleeding, infection, and rare nerve injury.
The consent discussion should cover alternative diagnostic options, the possibility of non-diagnostic samples requiring repeat biopsy, and the implications of both benign and malignant results. Documenting this process, including the patient’s questions and understanding, is crucial for legal and billing compliance, supporting the accurate use of the CPT code.
The Biopsy Procedure Itself
The ultrasound-guided thyroid biopsy, often billed using CPT code 60008, begins with patient positioning for optimal visualization. Real-time ultrasound guides a fine-needle aspiration (FNA) needle into the targeted thyroid nodule.
The radiologist visualizes the needle’s path, minimizing risk to surrounding structures. Multiple passes are typically performed to collect an adequate sample for pathological analysis. Proper sample handling and preservation are vital for accurate results, directly impacting diagnosis and subsequent treatment decisions related to the procedure coded as 60008.
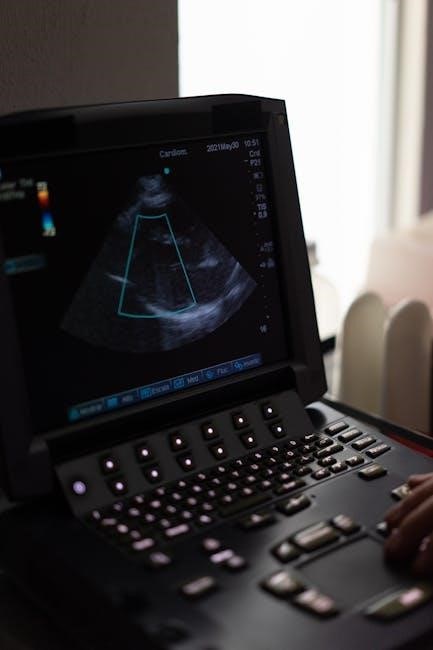
Ultrasound Guidance and Needle Placement
Ultrasound guidance is paramount during a thyroid biopsy, frequently coded as CPT 60008, ensuring precise needle placement within the suspicious nodule. The radiologist uses real-time imaging to visualize the thyroid and surrounding anatomy, avoiding critical structures like nerves and blood vessels.
Sterile technique is maintained throughout. The needle, typically a fine-gauge, is advanced under direct ultrasound visualization, confirming its position within the target lesion before aspiration. Accurate guidance maximizes sample adequacy and minimizes complications, directly impacting the success of the procedure billed under CPT code 60008.
Sample Collection and Handling
Following successful needle placement – a key component reflected in CPT code 60008 billing – sample collection begins. Gentle aspiration is performed to retrieve cells from the thyroid nodule. Multiple passes may be necessary to obtain an adequate sample for accurate cytological evaluation.
Collected samples are immediately expelled onto glass slides, smeared thinly, and fixed in alcohol for preservation. Proper labeling is crucial, linking the sample to the patient and specific nodule. The remaining material may be submitted in a fluid-based medium. Meticulous handling ensures diagnostic quality, justifying the procedure’s coding under CPT 60008.
Post-Biopsy Care
Post-biopsy care is essential, though generally straightforward, following procedures coded as CPT 60008. Patients are typically monitored briefly for any immediate complications like bleeding. A small bandage is applied to the puncture site.
Patients receive instructions regarding managing potential discomfort – usually mild – with over-the-counter pain relievers. They’re advised to avoid strenuous activity for 24 hours. While rare, signs of infection (redness, swelling, pus) warrant immediate medical attention. Follow-up appointments are scheduled to discuss biopsy results, ensuring appropriate care aligned with the initial CPT 60008 procedure.
Managing Discomfort and Bleeding
Following an ultrasound-guided thyroid biopsy, often billed using CPT code 60008, minor discomfort is common. Over-the-counter pain relievers, like acetaminophen or ibuprofen, usually suffice. A small amount of bleeding from the puncture site is also typical and can be controlled with gentle pressure and a bandage.
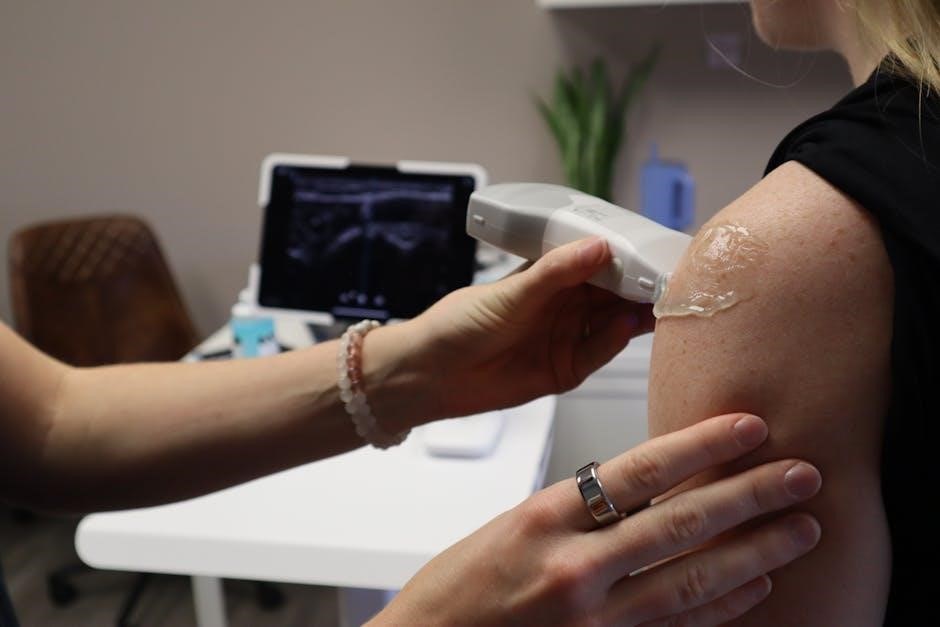
Patients should avoid strenuous activities for 24 hours to minimize bleeding risk. If significant bleeding occurs, or signs of infection develop (increased pain, redness, swelling, pus), immediate medical attention is crucial. Proper post-procedure care ensures optimal healing after the CPT 60008-coded biopsy.
Follow-up Instructions
After undergoing an ultrasound-guided thyroid biopsy – a procedure frequently coded with CPT 60008 – diligent follow-up is essential. Patients will typically receive biopsy results within one to two weeks, discussed with their physician. Further imaging or specialist referrals may be recommended based on these findings.
Regular thyroid function tests might be ordered to monitor overall thyroid health. It’s crucial to attend all scheduled appointments and promptly report any concerning symptoms, such as persistent pain, swelling, or difficulty breathing. Adhering to these instructions ensures comprehensive care post-CPT 60008 procedure.
Accuracy and Limitations of Ultrasound-Guided Biopsy
While ultrasound-guided thyroid biopsies, often billed using CPT code 60008, are highly valuable, they aren’t foolproof. False-negative results can occur, meaning cancer is present but missed during sampling. Conversely, false-positive results, though rarer, can lead to unnecessary anxiety and treatment.
Factors like small nodule size or sampling error can impact accuracy. It’s important to remember that a biopsy is a snapshot in time. Continued monitoring and clinical judgment, alongside appropriate CPT coding, are vital for optimal patient care and accurate diagnosis.
False-Negative Results
A false-negative result in an ultrasound-guided thyroid biopsy (often coded with CPT 60008) signifies cancer is present, yet the biopsy doesn’t detect it. This can stem from several factors, including inadequate sample size, sampling error – missing the cancerous area within the nodule – or the presence of a small, subtle malignancy.
Clinicians must consider this limitation, especially when initial biopsies are non-diagnostic. Repeat biopsies, coupled with careful clinical and radiological follow-up, are crucial. Accurate CPT coding reflects the procedure performed, but doesn’t eliminate the possibility of this diagnostic challenge.
False-Positive Results
A false-positive result following an ultrasound-guided thyroid biopsy (typically billed using CPT code 60008) indicates cancer cells are identified, but no malignancy actually exists. This can occur due to benign follicular hyperplasia mimicking cancer, inflammation, or laboratory errors during sample analysis.
Such results understandably cause patient anxiety and often lead to unnecessary further investigations, potentially including thyroid surgery. Careful pathological review and correlation with imaging findings are vital. Proper CPT coding ensures accurate record-keeping, but doesn’t preclude the possibility of this diagnostic error, necessitating clinical judgment.
The Impact of AI on Biopsy Decisions
Artificial Intelligence (AI) is increasingly influencing decisions regarding ultrasound-guided thyroid biopsies, often coded with CPT 60008. AI algorithms analyze ultrasound images to stratify nodule risk, potentially reducing unnecessary biopsies. By identifying nodules unlikely to be cancerous, AI minimizes patient anxiety and healthcare costs.
This technology doesn’t replace the radiologist, but serves as a valuable second opinion. Accurate CPT coding remains essential for billing, even with AI assistance. The goal is to refine biopsy indications, ensuring resources are focused on nodules with a higher probability of malignancy, improving diagnostic efficiency.
AI-Assisted Nodule Risk Stratification
AI significantly enhances nodule risk assessment before an ultrasound-guided thyroid biopsy (often billed using CPT code 60008). Algorithms analyze ultrasound features – size, shape, echogenicity, and margins – to predict malignancy risk. This stratification helps clinicians determine which nodules warrant biopsy, minimizing unnecessary procedures.
AI models are trained on vast datasets of thyroid ultrasound images, improving their accuracy over time. While AI doesn’t eliminate the need for expert radiologist interpretation and proper CPT coding, it provides a valuable tool for objective risk assessment, leading to more informed biopsy decisions and optimized patient care.
Reducing Unnecessary Biopsies with AI
AI is proving effective in decreasing the number of thyroid biopsies performed, impacting the utilization of procedures coded with CPT 60008. By identifying nodules with a very low probability of malignancy based on ultrasound characteristics, AI helps avoid invasive testing in many patients.
This reduction in unnecessary biopsies not only lowers patient anxiety and potential complications but also reduces healthcare costs. AI-powered tools offer a second opinion, assisting radiologists in confidently ruling out benign nodules, thus optimizing resource allocation and ensuring appropriate use of CPT codes for truly suspicious cases.
New Clinical Guidelines for Biopsy
Recent clinical guidelines aim to refine the criteria for thyroid biopsies, potentially influencing the frequency with which CPT code 60008 is utilized. These updated protocols focus on more precise risk stratification, reducing unnecessary procedures and ensuring biopsies are reserved for nodules with a higher likelihood of malignancy.
Specifically, new guidelines for pediatric patients, developed through studies like those at Loyola Medicine, offer a more targeted approach. This means fewer children undergo biopsies, impacting billing with CPT 60008. The overall goal is to improve diagnostic accuracy and minimize patient harm while maintaining appropriate coding practices.
Guidelines for Pediatric Patients
New clinical guidelines, stemming from research like Dr. Jennifer Lim-Dunham’s work, are significantly impacting biopsy decisions in pediatric cases, and consequently, the application of CPT code 60008. These guidelines prioritize identifying children genuinely at risk for thyroid cancer, reducing unnecessary procedures and associated anxiety.
The focus is on refined ultrasound criteria, allowing radiologists to more accurately assess nodule characteristics. This targeted approach minimizes the number of biopsies performed, potentially lowering overall healthcare costs and improving patient care. Accurate documentation supporting the use of CPT 60008 remains crucial for appropriate reimbursement.
Reducing Needless Biopsies in Adults
Experts are framing new clinical guidelines aimed at curbing unnecessary thyroid biopsies in adults, directly impacting the frequency with which CPT code 60008 is utilized. A significant portion of adults – up to two-thirds – have thyroid nodules, most of which are benign. These updated guidelines leverage improved ultrasound assessment and, increasingly, artificial intelligence (AI) to refine risk stratification.
By more accurately identifying nodules unlikely to be cancerous, clinicians can avoid invasive procedures. Proper documentation justifying the medical necessity for a biopsy, and therefore the use of CPT 60008, remains essential for billing and reimbursement purposes.
Billing and Coding Considerations
Accurate billing for ultrasound-guided thyroid biopsies hinges on correct CPT code application, primarily 60008. Comprehensive documentation is paramount, detailing the clinical indication, ultrasound findings necessitating the biopsy, and the procedure itself. Modifiers, such as -59 or -26, may be required to accurately reflect the services rendered and avoid claim denials.
Reimbursement policies vary among payers, demanding strict adherence to coding guidelines. Proper coding ensures appropriate compensation for the physician’s expertise and the resources utilized during the procedure. Understanding these nuances is crucial for healthcare facilities performing these biopsies.
Documentation Requirements
Thorough documentation is essential when billing for an ultrasound-guided thyroid biopsy using CPT code 60008. Records must clearly state the medical necessity, including palpable nodule characteristics or imaging findings prompting the procedure. Detailed ultrasound reports, outlining nodule size, composition, and suspicious features, are crucial.
The documentation should also reflect needle placement guidance, the number of passes performed, and sample adequacy. Any modifiers used (e.g., -59) must be justified. Complete and accurate records support appropriate reimbursement and demonstrate the quality of care provided during the biopsy process.
Reimbursement Policies
CPT code 60008, for ultrasound-guided thyroid biopsy, faces varying reimbursement policies among payers. Medicare and private insurers generally cover the procedure when medically necessary, supported by appropriate documentation demonstrating clinical indications like suspicious nodules. However, coverage can depend on specific criteria, such as nodule size and ultrasound characteristics.
Payers may scrutinize modifier usage, particularly -59 for distinct procedural services. Accurate coding and detailed reporting are vital for successful claims processing. Staying updated on individual payer guidelines and pre-authorization requirements is crucial to avoid denials and ensure timely reimbursement for ultrasound-guided thyroid biopsies.